by Thorsteinn Siglaugsson, Daily Sceptic:
I have previously written about a tendency by medical study authors to downplay their results if they don’t conform with the official narrative regarding the COVID-19 vaccines. A study done in Iceland and published last summer found that double-vaccinated individuals were 42% more likely to become reinfected than others. But in their conclusions the authors called this just a “slightly higher” probability.
Now, a new study is out, published in the BMJ, that deals with female menstruation problems following vaccination. Nothing to worry about, according to mainstream media reporting. Indeed, in their conclusions the authors say:
TRUTH LIVES on at https://sgtreport.tv/
Weak and inconsistent associations were observed between SARS-CoV-2 vaccination and healthcare contacts for bleeding in women who are postmenopausal, and even less evidence was recorded of an association for menstrual disturbance or bleeding in women who were premenopausal. These findings do not provide substantial support for a causal association between SARS-CoV-2 vaccination and healthcare contacts related to menstrual or bleeding disorders.
No reason to worry – really? Let’s take a look at the results section now:
2,580,007 (87.6%) of 2,946,448 women received at least one SARS-CoV-2 vaccination and 1,652,472 (64.0%) 2,580,007 of vaccinated women received three doses before the end of follow-up. The highest risks for bleeding in women who were postmenopausal were observed after the third dose, in the 1-7 days risk window (hazard ratio 1.28 (95% confidence interval 1.01 to 1.62)) and in the 8-90 days risk window (1.25 (1.04 to 1.50)). The impact of adjustment for covariates was modest. Risk of postmenopausal bleeding suggested a 23-33% increased risk after 8-90 days with BNT162b2 [Pfizer] and mRNA-1273 [Moderna] after the third dose, but the association with ChAdOx1 nCoV-19 [AstraZeneca] was less clear. For menstrual disturbance or bleeding in women who were premenopausal, adjustment for covariates almost completely removed the weak associations noted in the crude analyses.
So, actually significant risk for postmenopausal even after adjustments, but for premenopausal the “weak associations” were removed after adjustment for covariates. Why those huge adjustments? Before adjustment they found statistically significant increases of up to 44% – but that top figure was ‘adjusted’ away to just 4% (see Table 3). Yet even after these heroic adjustments there was still a 25% increase in menstrual disturbance following the first dose.
Anyhow, let’s look at the actual numbers by product for postmenopausal.
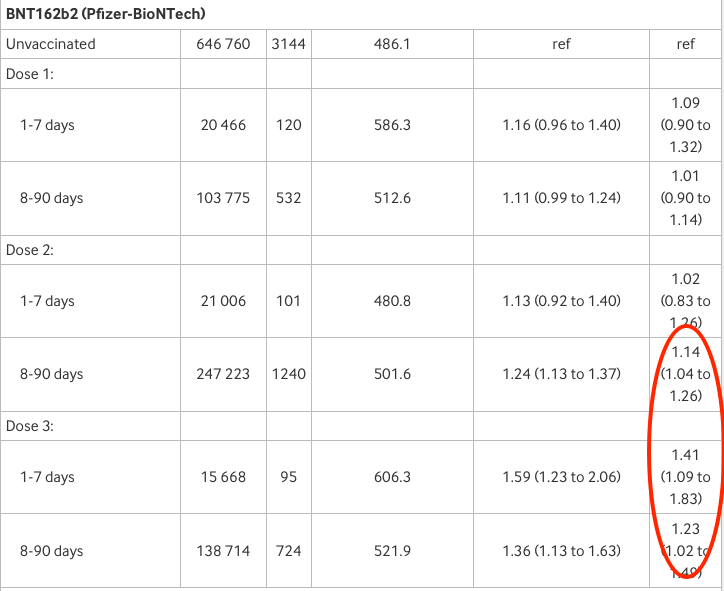
First Pfizer: adjusted risk (right-hand column) is 1.41 or 41% higher than the unvaccinated after 1-7 days from the third dose and 1.23 or 23% higher after 8-90 days. Both are statistically significant. “Weak and inconsistent?” Really?
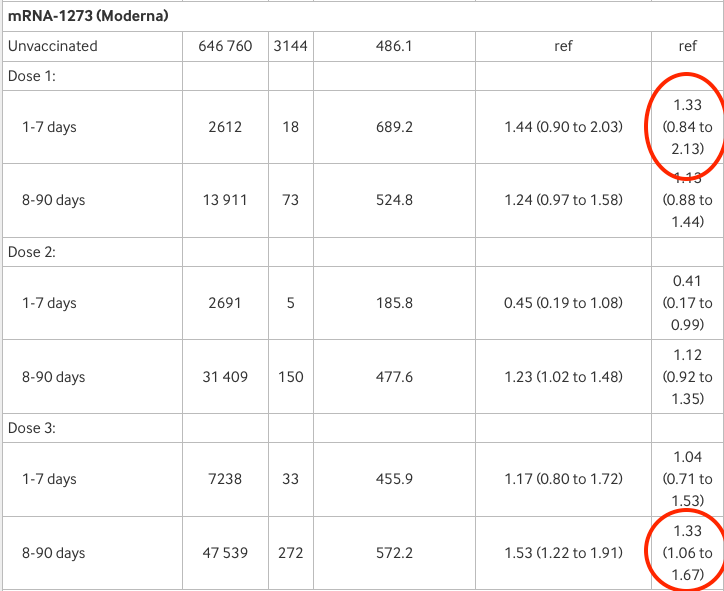
Now for Moderna: adjusted risk is 1.33 or 33% higher than unvaccinated after 1-7 days from first dose and also 8-90 days after the third (the latter is statistically significant). Again, “weak and inconsistent”?
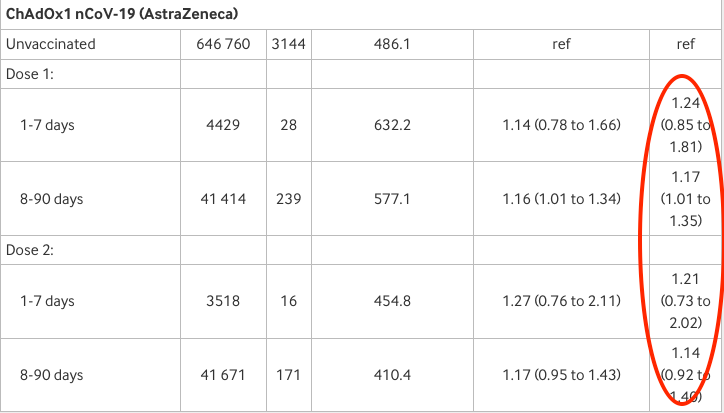
Finally AstraZeneca: adjusted risk is 1.24 or 24% higher than the unvaccinated 1-7 days after the first dose and 1.21 or 21% higher than unvaccinated after the second (though neither result is statistically significant).
Last October, the European Medicines Agency finally recommended adding menstrual problems to the already long list of COVID-19 vaccine side-effects. It was about time, after the flood of reports from women. The results of the new study reinforce those concerns, as shown above.
The question that remains is why the glaring discrepancy between the actual results and the authors’ conclusions?
The authors know full well that most journalists neither read nor understand scientific studies; they know how their highest ideal of verification is appeal to authority (‘the authors say, therefore it is true’). Every scientist knows this. Therefore, it is the authors’ responsibility to correctly portray and highlight their actual findings. But instead they try to hide them.



